Simulation Is About to Get Much More Real
By Lynn Burbank, DNP, MSN, RN, APRN, Global Senior Manager for Infection Prevention, Medical & Scientific Affairs, at Olympus Corporation of the Americas.
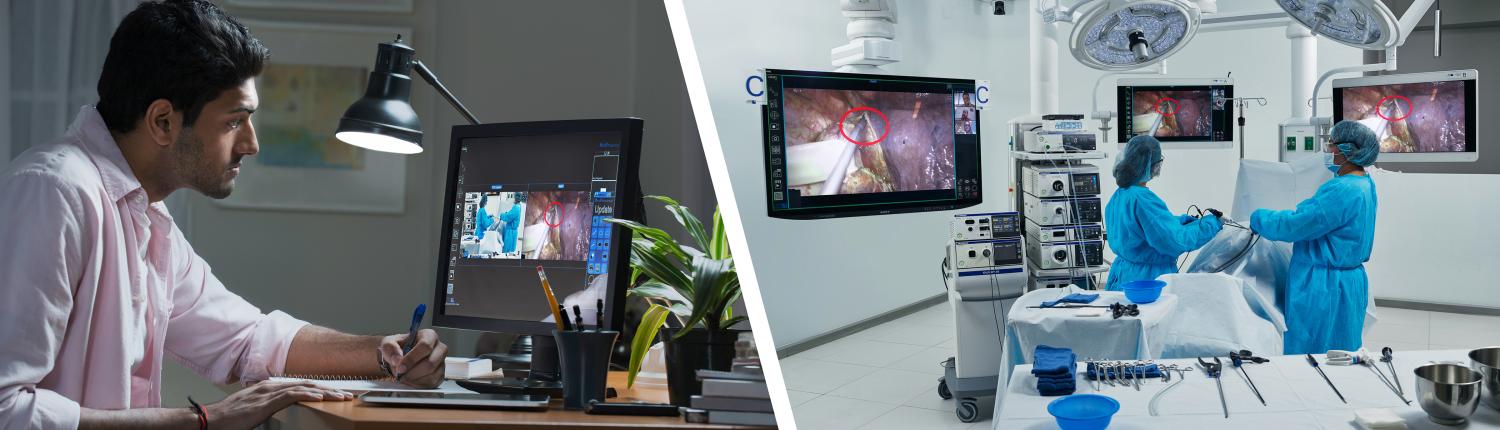
COVID-19-related restrictions on in-class learning have limited access to procedure spaces and created a demand for alternatives such as virtual clinical education. Remote participants such as students, fellows, and mentors need a remote access tool that provides in-room and clinical context video and audio communications—a tool that is much more robust than the typical video teleconference platform.
A telecollaboration platform robust enough for medical purposes needs to provide:
- An information-rich display reflecting multiple modalities such as ultrasound, live and reference lateral views, and views of the physicians’ hands outside the body
- High-fidelity audio and video showing both the room context and the clinical source
- Telestration capabilities allowing students to engage with the physician during the procedure
- A security architecture that supports compliance with the Health Insurance Portability and Accountability Act (HIPAA)
- A remote user experience identical to that of being in a hospital OR or procedure room, to ensure a seamless transition from looking in on simulation cases to live cases.
A recent article published in the Journal of NeuroInterventional Surgery describes a case in which a physician in the US was supervised remotely by another physician in Canada while placing a new device for the treatment of brain aneurysms. Cloud-based software provided real-time, audiovisual streaming from the OR to the expert physician in Canada who was able to supervise the first US use of a new type of flow-diverting implant. The article concludes that this successful teleproctoring case could eliminate the need for in-person supervision.
Just as Laerdal’s SimMan® and simulation-based education changed the face of medical and nursing education in 2001 by creating resuscitation simulation mannequins with pulse points, pupil dilation, and other lifelike features, so too can telecollaboration tools. These tools provide an in-room experience for remote participants who cannot be present in the OR.
Using telecollaboration, students can be brought into a procedure space from across the organization or around the world. The COVID-19 pandemic has made it essential to provide this type of technology to advance education and training in the latest surgical techniques and best practices.
Find out more about MedPresence, the Olympus telecollaboration platform.